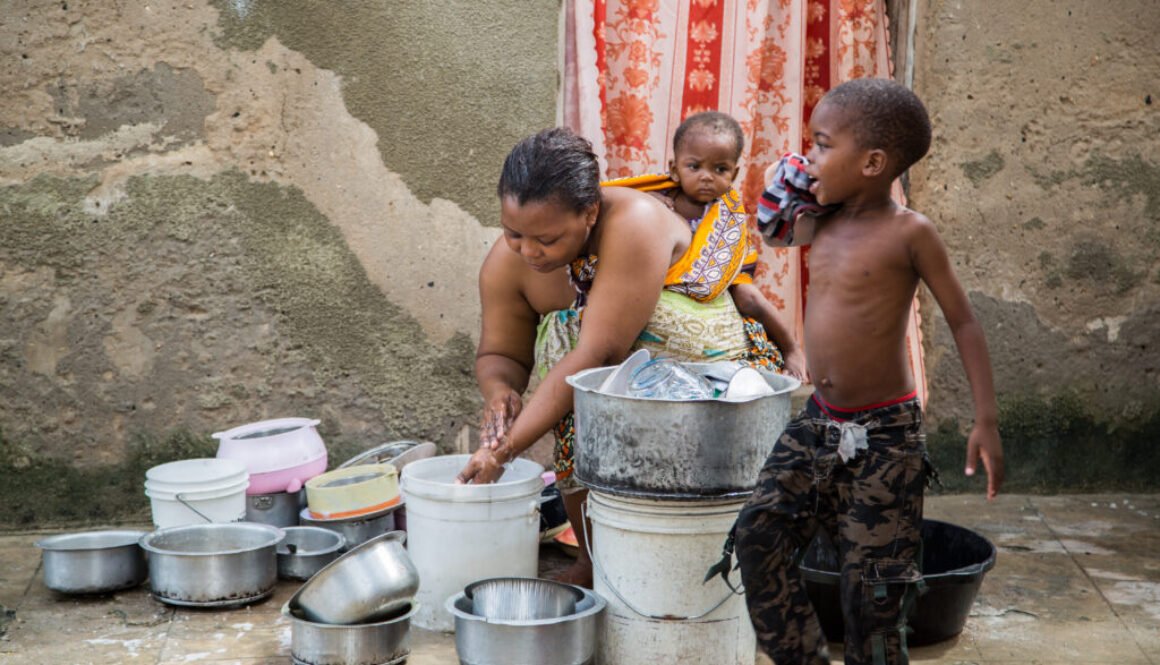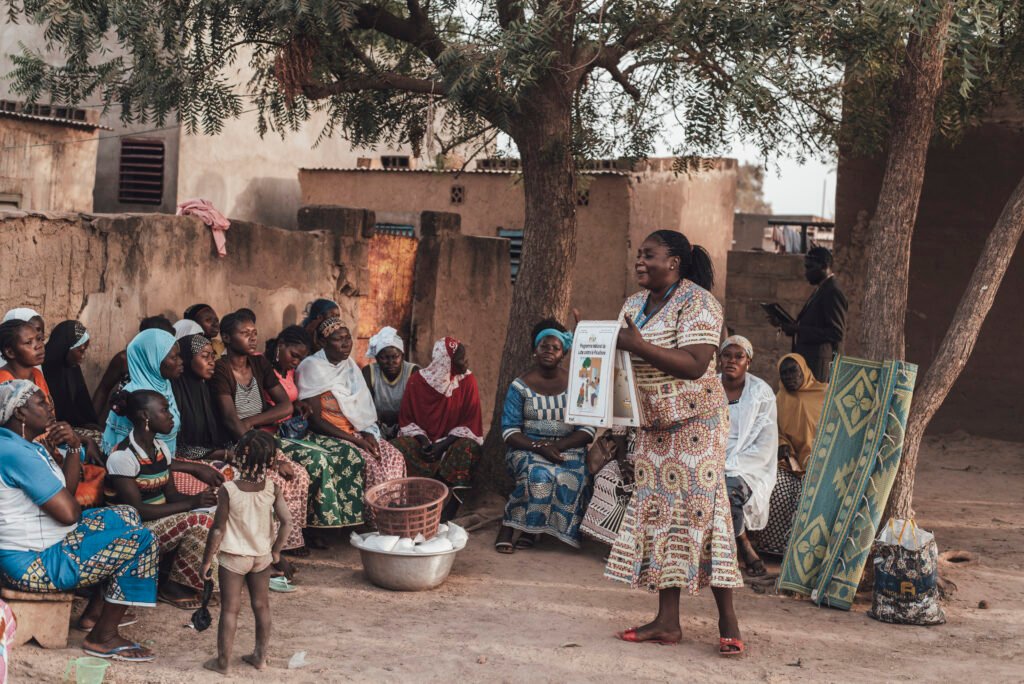Antibiotics and childhood illness: Everyday realities of caregivers in Nairobi’s informal settlements
In this blog Sammy Gachigua and Anne Ngunjiri describe both the crucial role of caregivers in acting on AMR and the realities of life in informal settlements which make medicine use fraught.
Walking through Nairobi’s informal settlements, you cannot miss the resilience of families who raise young children in the midst of immense challenges. Mothers balance small businesses with childcare, fathers juggle daily hustles to feed their households, and grandparents step in when parents are absent. In these crowded environments, where diarrhoea, malaria, coughs, and flu are part of daily life, caregivers are constantly making decisions about when and how to treat illness. At the centre of these choices is the use of medicines, especially antibiotics, which are often seen as the quickest route to recovery.
Yet behind each packet of tablets bought from a chemist or handed out at a health centre lies a complex web of poverty, health system gaps, and cultural practices. We spoke to caregivers of children under five years old in Kibera and surrounding areas to understand these everyday realities. Their stories reveal how antimicrobial use is shaped by the harsh conditions of informal settlements, and how this, in turn, fuels the threat of antimicrobial resistance (AMR).

For caregivers, the health of young children is a constant concern. Diarrhoea, coughs, malaria, and flu-like symptoms dominate conversations. Overcrowded homes, unsafe water, and poor sanitation mean infections spread quickly. A caregiver explained that diarrhoea is frequent because “the environment is dirty” and children are often exposed to sewage and contaminated water. Another parent added that coughs and chest problems worsen whenever the weather changes, forcing children to remain indoors. In these conditions, illness is not an occasional event but part of everyday life. Caregivers spoke of being in and out of hospitals or chemists several times a month. Some rely on public facilities like Otiende Health Centre, while others seek care at smaller NGOs or private clinics nearby.
But hospital visits are not always straightforward. Long queues, stock-outs of essential medicines, and the costs of transport often push families toward pharmacies as their first option.
(Insert image: A crowded waiting area outside a government clinic, with mothers holding babies)
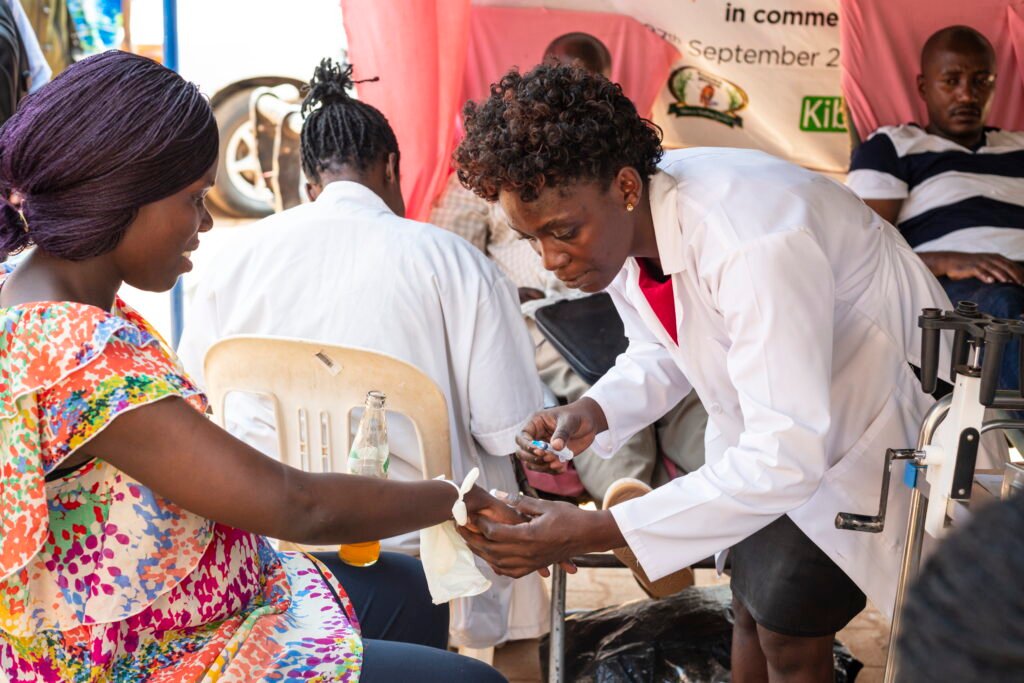
While hospitals are valued for diagnosis and testing, chemists play a much larger role in actual treatment. Parents repeatedly described situations where they go straight to the pharmacy, explain symptoms, and leave with medicine.
One father admitted that when his child falls ill, he often just buys medicine worth fifty shillings to try at home first before considering a hospital visit. Caregivers view pharmacies as accessible and flexible – they are nearby, they do not require consultation fees, and they allow purchases in small amounts. One mother noted that she might buy just two or three tablets of an antibiotic because she cannot afford the full dose. Others described keeping medicines like Panadol at home for emergencies, giving them to children at night when health facilities are closed.
This practice of partial dosing, self-prescribing, and relying on advice from chemist attendants rather than trained clinicians creates major risks for AMR. But for caregivers struggling with poverty and urgent childcare needs, it feels like the only practical solution.
Health choices have financial costs
At the heart of antimicrobial use decisions is money. Caregivers often described weighing the severity of a child’s illness against the cost of treatment. A grandmother caring for her disabled grandchild explained that she sometimes delays treatment until she can borrow money, even if the child has been unwell for days. Another parent said that hospital visits quickly become unaffordable because, even with government insurance schemes, many drugs are unavailable and must be bought out-of-pocket.
Families often rely on informal support systems — borrowing from neighbours, joining community savings groups, or depending on small earnings from odd jobs to cover the cost of drugs. The constant trade-offs mean that children may not always complete full courses of medicine. As one respondent admitted, once symptoms improve, medicines are often stopped early to save the remaining tablets for the next illness.
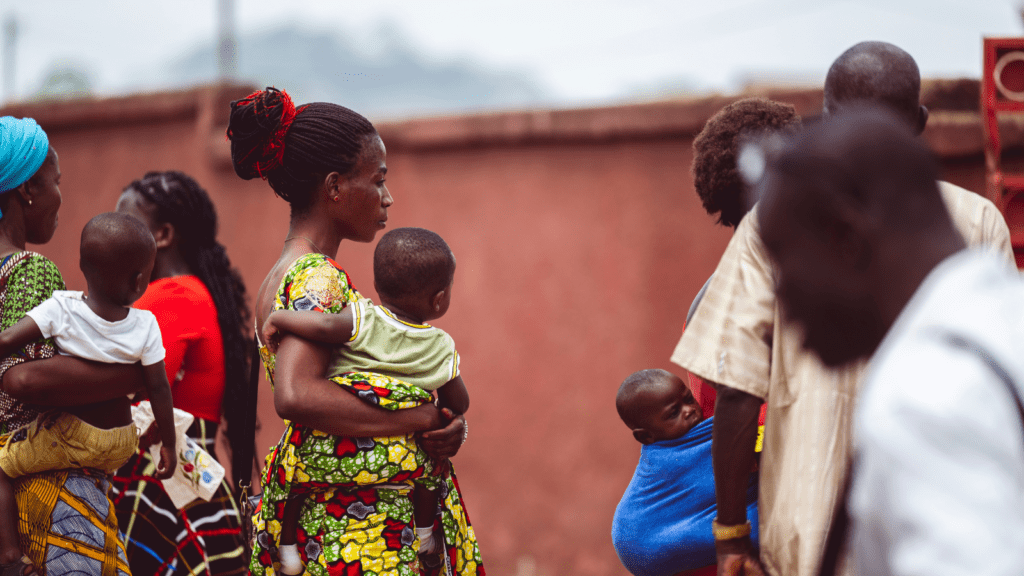
Interestingly, some caregivers showed awareness of the idea that medicines can stop working if misused. One father explained that frequent use of malaria drugs in his home region had led to a point where “you don’t get cured anymore.” Another caregiver noted that overusing antibiotics could make them act “like poison in the body” instead of curing illness. But even when this awareness exists, it rarely changes behaviour because the immediate priority is making a sick child feel better quickly. The long-term risks of AMR are overshadowed by urgent financial and health pressures.
The voices of caregivers highlight an urgent truth: strategies to combat AMR cannot succeed without addressing the social and economic realities of families in informal settlements. Telling people to complete doses or avoid self-medicating will not work if medicines are unaffordable, unavailable, or only accessible in partial amounts.
Supporting caregivers means ensuring that public facilities are stocked with essential medicines, strengthening regulation of pharmacies, and creating health financing systems that truly reduce out-of-pocket costs. It also means recognising the gendered dynamics of care, where women are often the ones negotiating treatment decisions within households under tight economic constraints.
Most importantly, it means amplifying the voices of caregivers themselves. They understand better than anyone the daily struggles of keeping young children healthy in these environments, and their insights are crucial to designing solutions that are both effective and realistic.