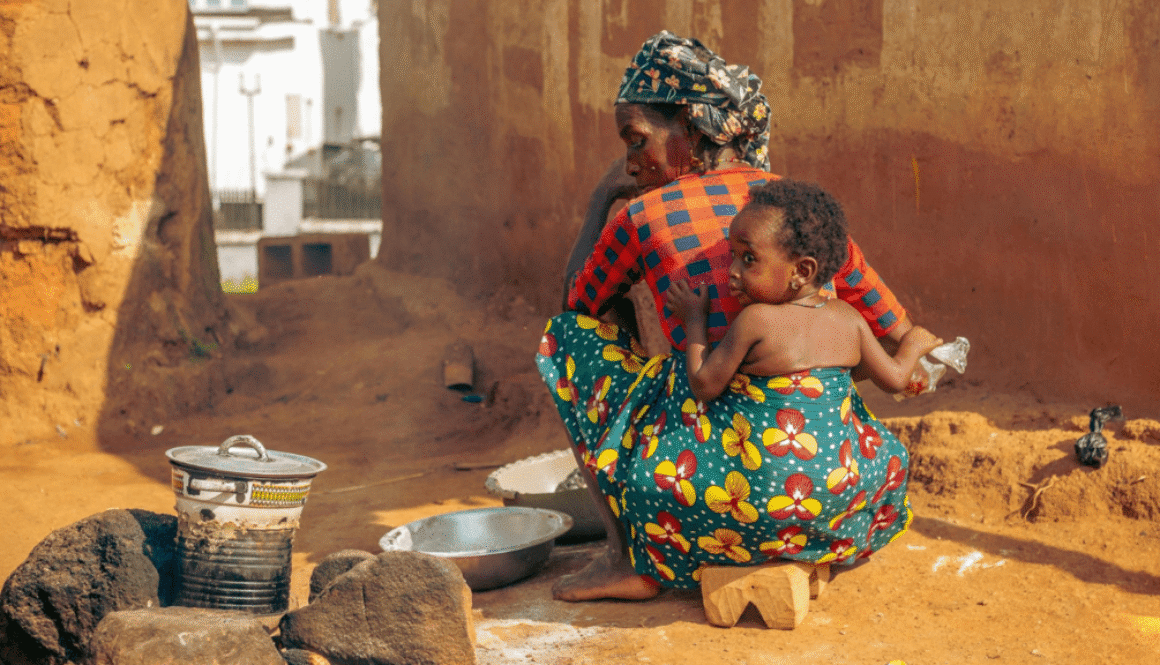Women as primary change agents in the AMR response in informal settlements
This blog, written by Sammy Gachigua and Anne Ngunjiri explores how women are acting as change agents in the response to Anti-Microbial Resistance in Kenya’s informal settlements. Despite the challenges they are making tough decisions and caring for their families with very little knowledge of AMR or support to alter the environmental and structural factors that drive vulnerability.
Walking through the crowded lanes of Nairobi’s informal settlements, one immediately notices the rhythm of daily life. Clothes hang from wires strung between tin houses, the air carries the scent of frying chapati mixed with smoke from charcoal stoves, and children weave in and out of narrow alleys, their laughter punctuated by the cries of infants strapped to their mothers’ backs. Amidst all this energy and struggle, there is an unspoken reality: illness is never far away.
In these settlements, sickness is woven into daily life. Poor drainage, open sewers, piles of rubbish, and unsafe water create constant health risks. Malaria, diarrhoea, chest infections, and tuberculosis are common, and children fall sick frequently. Yet, when illness arrives, it is women who respond first. They are the ones who notice a fever at night, who decide whether to try a home remedy or rush to the chemist, and who balance the impossible choices of paying for medicine or saving for food.
This blog draws on conversations with young mothers, older caregivers, and grandmothers in Nairobi’s Raila settlement, conducted through focus group discussions and in-depth interviews. These women’s voices reveal their central role in tackling antimicrobial resistance (AMR) — not as abstract policymakers or scientists, but as everyday change agents whose decisions directly shape how antibiotics are used in homes and communities.
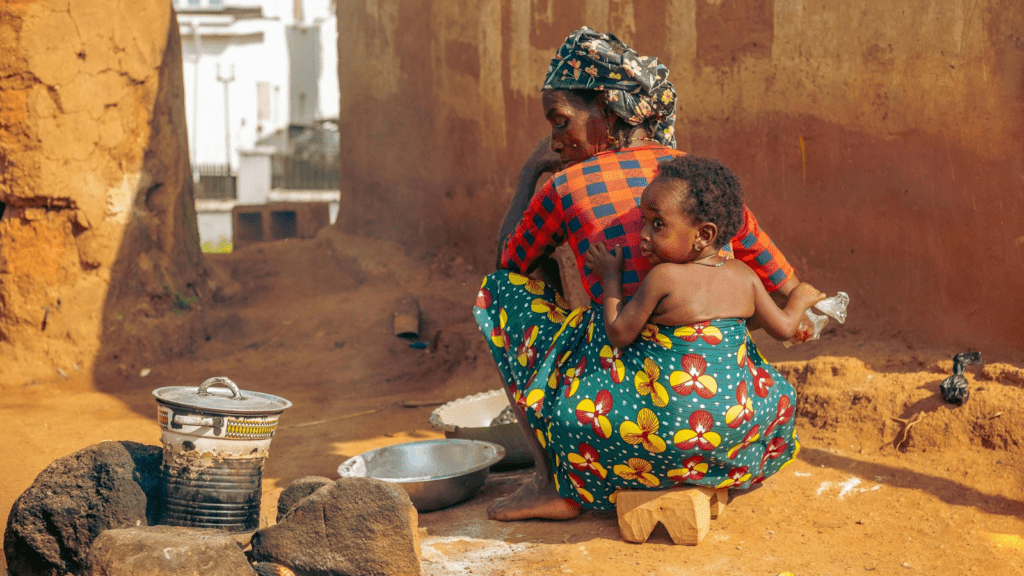
Women as first responders in the face of illness
For families in Raila, illness is expected, almost normalised. When women spoke about the most common conditions, they listed diarrhoea, malaria, fever, fungal infections, and coughs as part of daily reality. These diseases are not accidents. They stem from the environment: unsafe water, blocked drainage, poor toilets, and overcrowding.
One woman captured it simply when she said, “The environment is dirty… like diarrhoea, dirty water, sewage, just that”. Her words reflected what anyone walking the settlement would see. During rainy seasons, dirty water flows freely through alleys, carrying rubbish into homes. Toilets are shared by many families, often without water, and some residents pay to use them. As another mother explained, “Sometimes we have to pay to use a toilet, ten shillings per person. If you have five people at home, that’s fifty shillings in a day. Many can’t afford that.”
The health consequences are predictable. Children fall sick with diarrhoea, stomach aches, and fevers. Coughs and chest infections spread quickly in crowded rooms. Mothers and grandmothers described watching helplessly as infections returned again and again, sometimes responding to medicines, other times not.
In this context, women play a role that is both intimate and powerful. They are the frontline health responders in their homes. They observe symptoms, interpret signs, and decide the next step.
The pattern is familiar: if the illness seems mild, a woman may give painkillers from a shop or herbal remedies passed down by older generations. If it worsens, she may buy antibiotics at the chemist, sometimes a few tablets at a time rather than the full dose because of cost. Only when the sickness persists or becomes severe does she take the patient to the hospital.
One young mother explained her routine: “When someone is sick at home, I first assess the signs. Sometimes I buy medicine from the chemist to help for a while, then the next day I take them to hospital.”
For women with young children, this role is even more pronounced. They stay alert to every cough, fever, or bout of diarrhoea. One participant described rushing her child to hospital at night, despite neighbours warning her it was witchcraft and that injections could kill him. She followed her instincts, and her child survived.
Such decisions are rarely made lightly. They involve weighing risks, money, distance, and time. But they are decisions women make daily, often under enormous pressure.
Power, agency, and exclusion in access to medicine and use
Inside households, women hold both power and vulnerability. They often make final decisions about their children’s health. They are the ones who wake at night when a child’s fever spikes, who walk to the chemist, and who insist on finishing doses. But they also face barriers.
One young mother recalled, “I can see my child is sick, but my husband says it’s not serious since he already bought medicine last week. It hurts because I know the child needs help.”
Another laughed wryly as she explained that while she decides for herself and her children, her husband makes his own choices: “For me and the children, I decide. But for my husband, he decides by himself. Him and drugs – it’s tricky.”
Women bear the responsibility for health but do not always have the authority or resources to act freely. This tension complicates their role as agents of change but also underscores their resilience in pushing forward despite limitations.
When women spoke about how they use medicines, a pattern emerged. Many are careful, following prescriptions and ensuring children take full doses. But financial hardship often forces shortcuts. Some stop treatment early once symptoms improve. Others share leftover antibiotics with neighbours whose children have similar illnesses. Still others reuse medicines from previous prescriptions when symptoms appear familiar.
These practices, while understandable in context, increase the risk of AMR. One participant explained, “I had the same symptoms as last time, so I just took the remaining medicine hoping it would help me again.”
Another admitted, “If my friend complains of a headache and I have Panadol, I give her. I cannot deny her.”
At the same time, women are not unaware of resistance. Several spoke of medicines that seemed to stop working. “We were told that when you use medicines frequently, your body becomes resistant. You take the medicine but don’t get better,” said one.
This awareness, however, collides with the realities of poverty. Knowing the risks does not always translate into safer behaviour when survival is at stake.
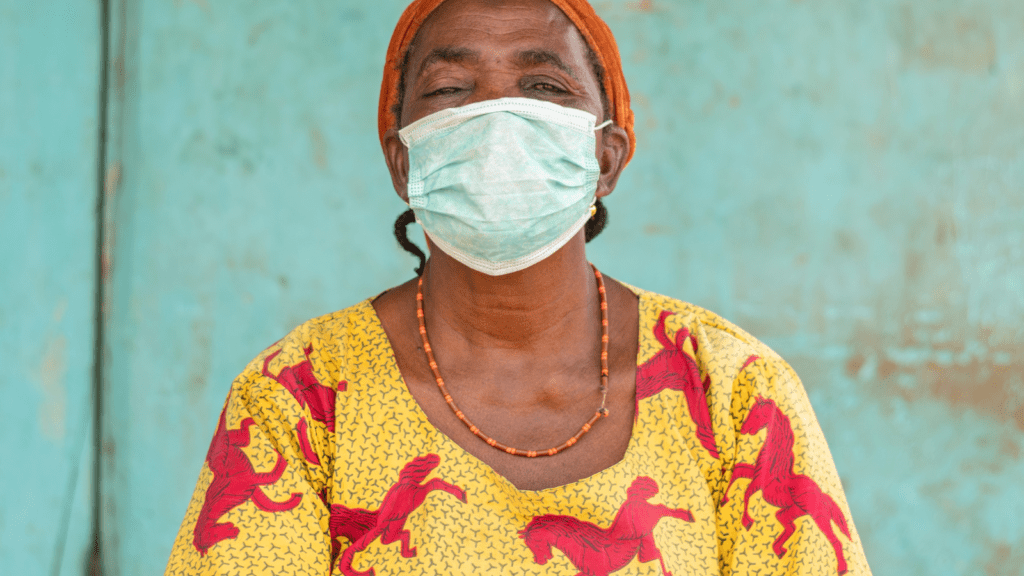
Women find ways to keep their families alive and healthy despite daunting barriers. They carry children to hospitals on their backs, take on casual work to pay for prescriptions, and support each other through community networks.
They are also clear about what they want. They ask for health facilities closer to home, for doctors who arrive on time, for medicines that do not run out, for affordable services, and for respect in how they are treated.
One woman summarised it powerfully: “If services could be improved, if medicines were available, if water was treated – it would help reduce diseases.”

Why women must be at the centre
The stories from Raila show that AMR is not an abstract scientific issue. It is lived daily in informal settlements, shaped by decisions women make under pressure: whether to give a child antibiotics, whether to share leftover medicine, whether to finish a course despite the cost.
These decisions, repeated across thousands of households, determine whether resistance grows or slows. Women are not just caregivers; they are frontline health workers in their own right. Recognising this and supporting them with affordable healthcare, accessible medicines, and better information is essential.
If we are serious about tackling AMR, we must place women at the centre of the response. They already are the change agents. What they need is support, recognition, and respect.