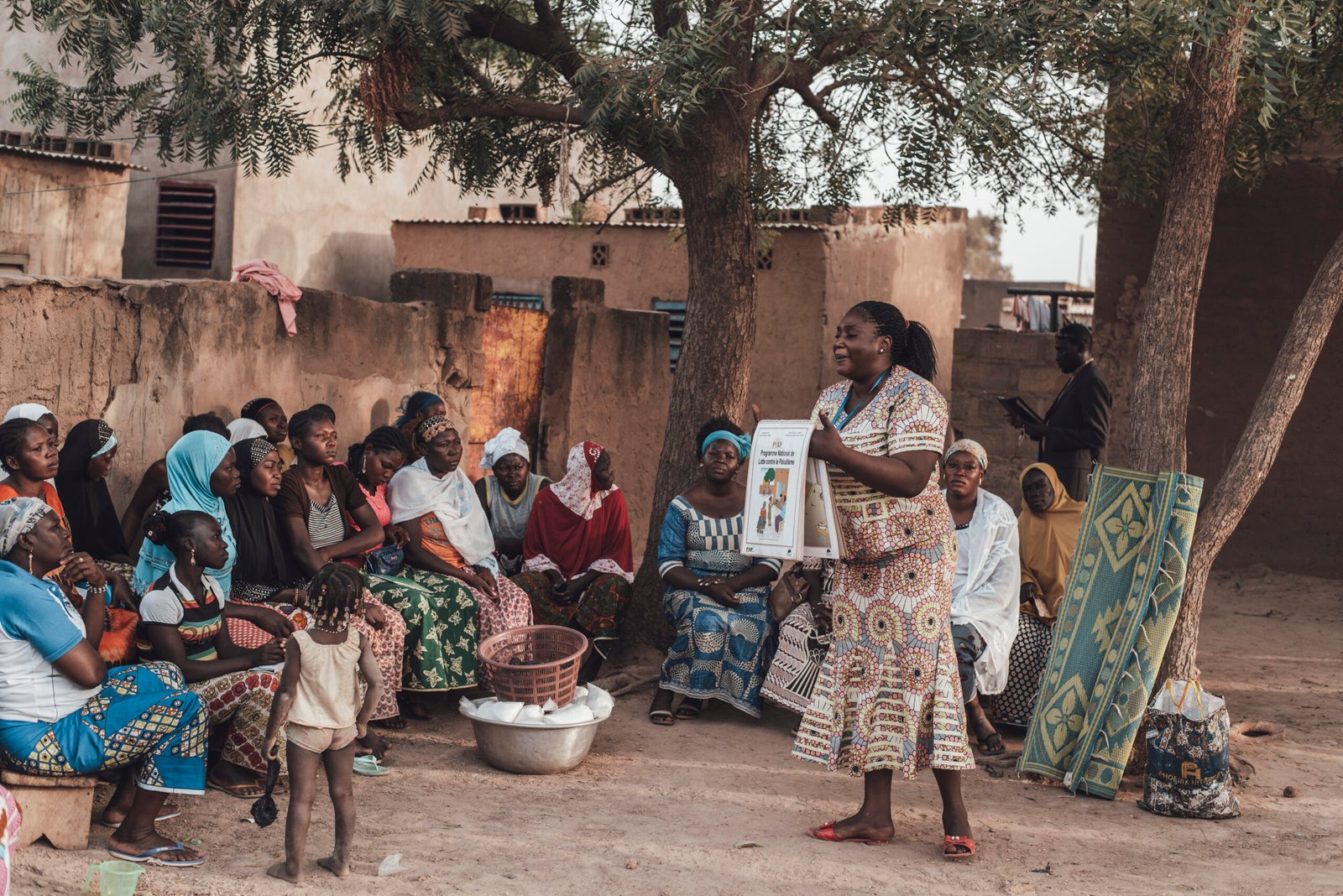This blog by Sammy Gachigua and Anne Ngunjiri explores how community health workers play a key role in health information on AMR and connecting very vulnerable communities to the health system by creating trusting relationships. It suggests ways in which this role could be formalised and supported by the state.
When you step into Nairobi’s informal settlements, you are struck by how much life happens in tight, unplanned spaces. Narrow paths wind between corrugated iron homes, children chase each other barefoot through alleys, and vendors call out from makeshift stalls. Beneath the vibrancy, however, illness is an ever-present reality. Dirty water pools in open drains, toilets are overcrowded or inaccessible, and the air carries dust and smoke that fuel persistent coughs.
In such settings, health is not only managed in hospitals or clinics. It is managed at home, in conversations between neighbours, and in the quiet interventions of people who are rarely recognised in formal health systems — the Community Health Promoters (CHPs).
These CHPs are local men and women chosen by their communities to support households with health education, referrals, and follow-up. They walk door to door, checking in on pregnant women, monitoring newborns, following up on sick children, and reminding families to complete treatments. They are volunteers, often juggling their own survival with the responsibility of caring for up to 100 households each. And yet, despite being the bridge between health facilities and the communities they serve, their role in combating antimicrobial resistance (AMR) remains almost invisible.
Life on the frontline of illness – What CHPs actually do
The daily reality in informal settlements is that illness is constant. Families talk of diarrhoea, malaria, flu, and skin conditions as part of normal life. Outbreaks of cholera sweep through after the rains, and coughs linger for months in damp, crowded homes. Poverty shapes how people respond. For many, a hospital visit is the last resort – medicines are costly, transport is costly, and queues are long. Public facilities often run out of drugs, leaving families with prescriptions they cannot afford to fill. Instead, residents turn to local chemists. They buy antibiotics or painkillers in small quantities, often just two or three tablets at a time. A CHP explained that people stop treatment when symptoms improve, saving the rest for another day or for another family member with similar complaints. In the absence of money, medicine is rationed like food – stretched as far as possible, even when it means incomplete treatment.
In this fragile system, CHPs become the quiet custodians of health. They are assigned households, but their real work is relational: building trust, offering advice, and persuading families to seek care when they would otherwise delay. They teach handwashing, check immunisation cards, and encourage families to go for antenatal visits. They explain how to take medicine properly, why finishing antibiotics matters, and when to return to hospital.
Their work is critical in the health of the community. One CHP described herself simply as, “the bridge between the hospital and the household.” Without her, she said, many neighbours would never reach formal care. The trust they hold is critical. Families often confide in CHPs before they approach nurses or doctors, especially for sensitive conditions like sexually transmitted infections or reproductive health. They are seen not just as health promoters, but as neighbours who care, who listen without judgment, and who remain available long after hospital staff have gone home.
Barriers to medicine use
A recurring theme in conversations with CHPs is the way that people use medicines ‘improperly’. In the settlements, antibiotics are viewed as cure-alls, used for everything from headaches to stomach pain. Leftover medicines are shared among neighbours. Some parents store antibiotics in case a child falls sick at night. Others buy whatever the chemist suggests, sometimes without prescriptions.
CHPs spoke of families abandoning treatment after just two days when symptoms improved. They see people switching to herbal remedies if illness persists, or turning to traditional healers when modern medicines seem ineffective. Misconceptions are common. Some believe persistent illness is caused by witchcraft, while others think taking too much medicine makes the body “weaker.”
For CHPs, addressing these beliefs is part of their daily work. They remind families that unfinished treatment not only fails to cure the illness but can make medicines stop working in the future. They explain that what feels like poison in the body is actually resistance developing. One CHP put it plainly: “When you misuse antibiotics, it can turn into poison in the body. The illness will not go, and another one will emerge.”
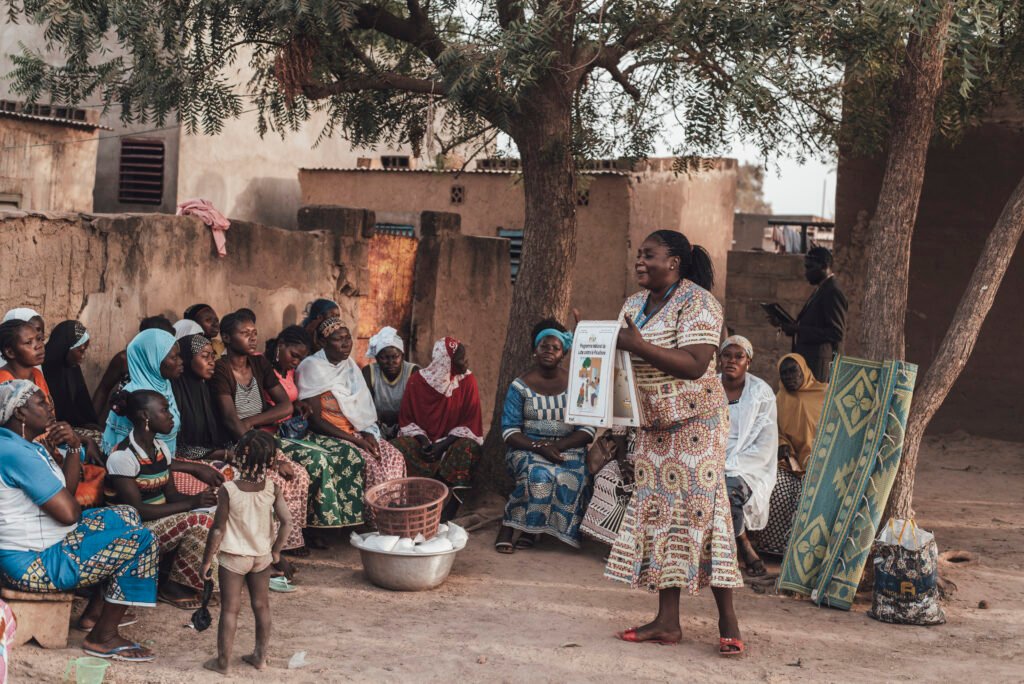
Knowledge without recognition
What is striking is how much CHPs already know about AMR, even if they do not always use that terminology. They see resistance not as a laboratory result, but as lived experience: medicines that used to work no longer do, coughs linger despite repeated treatment, and children relapse after partial courses of drugs. They connect these patterns with incomplete treatment and misuse, and they do their best to intervene with the limited tools they have.
Their approach goes beyond medicine. CHPs emphasise hygiene, clean water, and nutrition. They use local language, stories, and practical examples to make health advice relatable. They rely on persuasion rather than authority, often enlisting respected relatives or community elders to reinforce messages. In this way, they weave health education into everyday life, making it part of conversations rather than lectures.
Despite their dedication, CHPs face enormous challenges. Many households resist their advice, preferring the quick fix of buying drugs from a pharmacy. Some dismiss them as busybodies. Others suspect they are paid to disturb families, when in reality, CHPs receive little or no compensation.
The lack of medicines at government facilities undermines their credibility. When they encourage families to go to the hospital only for patients to be turned away with empty prescriptions, frustration builds on both sides. Trust erodes, not because of CHPs themselves, but because the system they represent feels broken.
In some cases, CHPs face outright hostility. They have doors slammed in their faces, are insulted, or accused of interfering in matters beyond their concern. Yet, despite the resistance, they keep going, driven by the belief that their work saves lives.
Witnessing AMR first-hand
CHPs may not call it AMR, but they recognise its signs. They hear constant complaints that medicines “no longer work.” They notice families trying the same drugs repeatedly without success. They see people turning to herbal remedies after antibiotics fail. They watch as amoxicillin, once effective for many illnesses, becomes less reliable.
Their response is pragmatic. They encourage families to return to hospital, accompany them when possible, and explain the link between misuse and ineffectiveness. They see themselves as educators as much as caregivers, fighting a quiet battle against resistance one household at a time.
The experiences of CHPs make it clear that any effort to address AMR in informal settlements cannot be confined to hospitals, policies, or laboratories. It must begin with the people who influence how medicines are used at household level and that means recognising CHPs.
They are not simply volunteers; they are frontline health workers operating in the hardest-to-reach communities. Yet they lack proper training on AMR, receive little material support, and are excluded from national strategies. Recognising them means equipping them with knowledge, ensuring their advice is backed by reliable access to medicines, and formally including them in AMR responses.
Most importantly, it means listening to them. CHPs provide a window into how communities actually use medicines, insights that policy papers or hospital records cannot fully capture. They are the missing link in the fight against AMR.
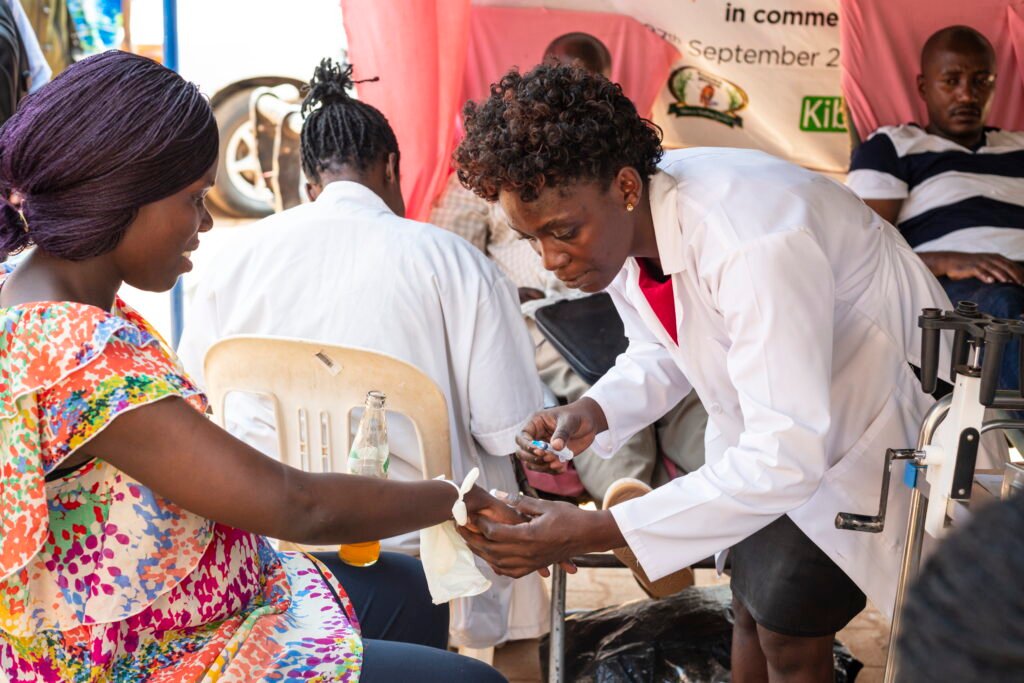
CHPs are already acting as change agents, but they are doing so quietly, often invisibly. If their role were formally recognised, supported, and integrated into AMR strategies, they could play an even greater part in preventing resistance.
By investing in their training, providing them with stipends or material support, and ensuring hospitals back up their referrals with reliable services, governments and donors can harness a resource that already exists in communities. Strengthening CHPs is not creating a new system. It is empowering the one that is already holding communities together.